Kirsch Waldenstrom's Macroglobulinemia Diary
By Steve Kirsch
This page describes my treatments and chronicles my blood measurements in response to treatment.
Related pages:
- Waldenstrom's macroglobulinemia: A new approach, I described my story.
- Waldenstrom's macroglobulinemia: Drug options describes my treatment philosophy and has info on various WM drugs.
- Waldenstrom's macroglobulinemia: Low dose Rituxan has some thoughts on alternate Rituxan dosings which I think should be tried.
Blood type: A+
| Date | Location | Pulse | BP | WBC | RBC | HCT | HGB | PLAT | RDW | POLY | %LYMPH | LYM ABS |
NEUT | MONO | IgA | IgG | IgM SPIE | IgM Serum |
Viscosity | Iron (serum) | Transferrin (TIBC) |
Transferrin Saturation |
Tot Prot |
Glucose | Globulin | Beta2 micro |
VLDL | LDL (calc) |
HDL | Trigly cerides |
Tot Chol |
Creatinine | CPK |
| Normal range | 3.8-9.2 | 4.2-5.6 | 38.4-48.2 | 13.2-16.7 | 155-410 | 11.5-14.8 | 49-79 | 11-38% | 1-3 | 1.7-6.7 | .3-.95 | 70-400 | 700-1600 | 50-300 | 40-230 | 1.4-1.8 | 49-181 | 230-450 | 20-60% | 6.0-8.0 | 70-100 | 2.0-5.0 | 609-2366 | <130 | >40 | <1.2 | 55-170 | ||||||
| 11/00 | Stanford | 1260 | 9.2 | ||||||||||||||||||||||||||||||
| 5/10/07 | Stanford | 9.0 | 5.2 | ||||||||||||||||||||||||||||||
| 5/14/07 | Stanford | 7.9 | 3.56 | 30.0 | 10.3 | 514 | 15.0 | 14.9 | 22 | 200 | 11 | 92 | 55 | 29 | |||||||||||||||||||
| 6/11/07 | Stanford | 2800 | 9.5 | ||||||||||||||||||||||||||||||
| 7/3/07 | Stanford | 9.5 | 3.72 | 31.9 | 10.6 | 524 | 15.0 | 14.4 | 2700 | 9.6 | 141 | 6.8 | 2590 | 1.2 | |||||||||||||||||||
| 9/11/07 | DFCI | 9.4 | 3.53 | 30.4 | 10.2 | 521 | 14.9 | 85 | 7 | 56 | 1100 | 3710 | 31 | 276 | 11 | 9.2 | 156 | 5.7 | 2700 | ||||||||||||||
| 9/12/07 | BWH | 14.09 | 3.32 | 28.3 | 9.4 | 601 | 13.8 | 9.0 | 156 | ||||||||||||||||||||||||
| 9/28/07 | Stanford | 113 | 96/65 | 9.5 | 3.61 | 31.0 | 10.4 | 564 | 15.2 | 17.3 | 10.2 | 84 | 6.4 | 1.0 | |||||||||||||||||||
| 10/31/07 | Stanford after 3 iron infusions | 103 | 85/56 | 8.8 | 3.71 | 32.0 | 10.8 | 579 | 15.3 | 14.6 | 3100 | 3770 | 2.8 | 26 | 152 | 17 | 10.1 | 133 | 7.1 | 1.1 | |||||||||||||
| 11/19/07 | DFCI | 10.1 | 3.66 | 32.0 | 10.7 | 609 | 15.5 | 71 | 17 | 49 | 1190 | 2830 | 4010 | 2.9 | 30 | 287 | 9.5 and 9.1 | 83 | 5.9 | 2700 | 13 | 58 | 21 | 68 | 93 | .9 | 25 | ||||||
| 11/28 | Stanford | 98 | 99/61 | ||||||||||||||||||||||||||||||
| 12/7/07 | Stanford | 48 | 1050 | 2700 | 3450 | 9.2 | 2948 | ||||||||||||||||||||||||||
| 12/9/07 | Stanford | 10.4 | 3.57 | 31.4 | 10.5 | 404 | 15.8 | 13.9 | |||||||||||||||||||||||||
| 12/11/07 | Stanford | 1.6 (before 3rd PP) | |||||||||||||||||||||||||||||||
| 12/12/07 10am | Stanford | 86/53 | 10.3 | 3.62 | 31.9 | 10.9 | 393 | 16.1 | 12.8 | 1.32 | 7.75 | 1.1 | 1.6 (after 3rd PP) | ||||||||||||||||||||
| 12/13/07 | Stanford 2 hours before Rituxan (start of CPR) |
21 | 361 | 1090 | 167 | 3.1 | .91 | ||||||||||||||||||||||||||
| 12/14/07 | Cytoxan given | ||||||||||||||||||||||||||||||||
| 12/18/07 11am |
Stanford 5 days after CPR |
9.6 | 3.02 | 26.4 | 9.1 | 460 | 15.9 | 6.6 | .64 | 8.7 | .26 | 1000 | 1.7 | 6.6 | 129 | 3.7 | 1.0 | ||||||||||||||||
| 12/26/07 | Stanford 13 days after CPR | 4.1 | 3.59 | 31.5 | 10.6 | 674 | 16.5 | 17.4 | .72 | 2.54 | 3000 | ||||||||||||||||||||||
| 1/16/08 | Stanford before first Rituxan 4x round |
115/75 | 8.2 | 4.01 | 35.8 | 11.8 | 482 | 15.3 | 15.5 | 1.28 | 5.88 | .96 | 47 | 795 | 3200 | 4290 | 3.0 | 10.3 | 151 | 7.1 | 1.04 | ||||||||||||
| 2/5/08 | Stanford before 3rd Rituxan infusion | 110/72 | 6.7 | 3.53 | 30.6 | 10.3 | 495 | 14.9 | 14.1 | .95 | 4.67 | .95 | 27 | 620 | 6270 | 4.8 |
| Date | Location | Pulse | BP | WBC | RBC | HCT | HGB | PLAT | RDW | POLY | %LYMPH | LYM ABS |
NEUT | MONO | IgA | IgG | IgM SPIE | IgM Serum |
Viscosity | Iron (serum) | Transferrin (TIBC) |
Transferrin Saturation |
Tot Prot |
Glucose | Globulin | Beta2 micro |
VLDL | LDL (calc) |
HDL | Trigly cerides |
Tot Chol |
Creatinine | CPK |
| Normal range | 3.8-9.2 | 4.2-5.6 | 38.4-48.2 | 13.2-16.7 | 155-410 | 11.5-14.8 | 49-79 | 11-38% | 1-3 | 1.7-6.7 | .3-.95 | 70-400 | 700-1600 | 50-300 | 40-230 | 1.4-1.8 | 49-181 | 230-450 | 20-60% | 6.0-8.0 | 70-100 | 2.0-5.0 | 609-2366 | <130 | >40 | <1.2 | 55-170 | ||||||
| 2/11/08 | Stanford to check SV again | 6.3 | 32. | 11.0 | 466 | 15.5 | 13.3 | .84 | 4.18 | 1.12 | 26 | 645 | 6320 | 4.5 | <130 | 11.4 | 73 | 8.4 | |||||||||||||||
| 2/14 | stanford 2 days after 1 PP | 19 | 414 | 3390 | |||||||||||||||||||||||||||||
| 2/25 | stanford 10 days after 2nd PP | 23 | 425 | 3910 | 2.6 | ||||||||||||||||||||||||||||
| 3/11 | Stanford | 7.0 | 3.82 | 34.2 | 11.9 | 379 | 14.9 | 16.6 | 1.16 | 4.95 | .76 | 29 | 482 | 4250 | 9.5 | 99 | 6.1 | 1.1 | |||||||||||||||
| 3/31/08 | Stanford | 12.6 | 2600 | 2.2 | |||||||||||||||||||||||||||||
| 4/23/08 | Stanford before 1st of 2nd round | 8.7 | 4.18 | 36.9 | 12.7 | 460 | 13.4 | 14.8 | 1.28 | 1.02 | 32 | 639 | 2390 | ||||||||||||||||||||
| 4/29/08 | Stanford before 2nd of 2nd round | 9.4 | 3.91 | 34.8 | 12 | 500 | 13.4 | 9.4 | .88 | 6.71 | 1.67 | 29 | 663 | 2380 | 2.1 | ||||||||||||||||||
| 5/6/08 | Stanford before 3rd of second round | 30 | 654 | 4660 | |||||||||||||||||||||||||||||
| 5/21/08 | el camino | 130/65 | 3.98 | 36.1 | 12.1 | 505 | 12.8 | 15.8 | 5.1 76.1% | 6.8% | 103 | 474 | 3522 | 9.4 | 171 | ||||||||||||||||||
| 5/29/08 | el camino | 3502 | |||||||||||||||||||||||||||||||
| 6/11/08 | el camino | 3118 | |||||||||||||||||||||||||||||||
| 6/24/08 | el camino | 2804 | |||||||||||||||||||||||||||||||
| 6/27/08 | el camino | 100 mg Rituxan infusion (my first) | |||||||||||||||||||||||||||||||
| 7/3/08 | el camino | 2347 | |||||||||||||||||||||||||||||||
| 7/21/08 | el camino | 2606 | |||||||||||||||||||||||||||||||
| 7/28/08 | el camino | 2249 | |||||||||||||||||||||||||||||||
| 8/04/08 | el camino | 2002 | |||||||||||||||||||||||||||||||
| 8/11/08 | el camino | 1848 | |||||||||||||||||||||||||||||||
| 8/25/08 | el camino | 1622 | |||||||||||||||||||||||||||||||
| 9/12/08 | el camino | 8.9 | 4.22 | 37.4 | 12.7 | 399 | 12.8 | 13.2 | 75.3 | 9.5 | 1622 | 8.2 | 141 | ||||||||||||||||||||
| 9/22/08 | el camino | 1607 | |||||||||||||||||||||||||||||||
| 10/29/08 | el camino | 1621 | |||||||||||||||||||||||||||||||
| 12/3/08 | el camino | 9.0 | 4.22 | 37.6 | 12.7 | 473 | 12.6 | 14.9 | 75.8 | 8.0 | 1809 | 7.9 | 144 | ||||||||||||||||||||
| 1/2/09 | el camino | 1868 | |||||||||||||||||||||||||||||||
| Date | Location | Pulse | BP | WBC | RBC | HCT | HGB | PLAT | RDW | ABS POLYS |
%LYMPH | LYM ABS |
NEUT % |
MONO % |
IgA | IgG | IgM SPIE | IgM Serum |
Viscosity | Iron (serum) | Transferrin (TIBC) |
Transferrin Saturation |
Tot Protein |
Glucose | Globulin | Beta2 micro |
VLDL | LDL (calc) |
HDL | Trigly cerides |
Tot Chol |
Creatinine | k/l |
| 1/20/09 | dfci | 8.6 | 4.0 | 35.7 | 12.1 | 443 | 13.4 | 70 | 8 | 36 | 868 | 1.82 (1.9) | 2540 (2880) | 1.5 | 8.6 | 200 | 4.5 | 2.4 | 1.1 | ||||||||||||||
| 1/28/09 | started enzastaurin clinical trial ()=covance lab results |
||||||||||||||||||||||||||||||||
| 2/9/09 | el camino | 1812 | |||||||||||||||||||||||||||||||
| 2/23/09 | dfci | 8.5 | 3.24 | 29.0 | 9.9 | 437 | 13.7 | 74 | 11 | 28 | 607 | 1.29 (1.1) | 1500 (1680)
|
1.1 | 7.0 to 7.7 | 86 | 4.0 | .9 | 2.53 | ||||||||||||||
| 3/10/09 | el camino | 7.9 | 3.82 | 33.4 | 11.4 | 500 | 13.3 | 16.8 | 1.3 | 72.6 | 8.8 | ||||||||||||||||||||||
| 4/2/09 | dfci | 8.9 | 3.84 | 33.4 | 11.3 | 393 | 13.7 | 39 | 818 | 1.58 (1.4) | 2290 (1910) | 8.0 | 3.16 | ||||||||||||||||||||
| 5/8/09 | dfci | 7.5 | 4.25 | 36.9 | 12.7 | 416 | 14.5 | 36 | 849 | 1.84 (1.9) |
2670 (2250) |
8.8 | 176 | 4.7 | 1.2 | ||||||||||||||||||
| 5/27/09 | el camino | 1908 | |||||||||||||||||||||||||||||||
| 6/4/09 | dfci | 10.3 | 3.96 | 34.2 | 11.9 | 404 | 14.3 | 7.11 | 23 | 2.37 | 37 | 757 | 1.73 | 2500 (2460) |
1.3 | 8.4 | 89 (i fasted) | 4.4 | 1.1 | 2.31 | |||||||||||||
| 6/5/09 | el camino | 1690 | |||||||||||||||||||||||||||||||
| 7/7/09 | dfci | 8.4 | 4.04 | 35.3 | 12.2 | 438 | 14.2 | 17 | 1.43 | 72 | 31 | 773 | 1.9 | 2480 | 1.7 | 8.3 | 143 | 4.6 | 1.1 | 2.00 | |||||||||||||
| 8/6/09 | dfci | 7.6 | 3.83 | 33.8 | 11.6 | 411 | 14.3 | 19 | 1.44 | 67 | 11 | 33 | 767 | 1.78 | 2320 | 1.5 | 8.0/8.3 | 134 | 4.3 | 1.1 | .942 | ||||||||||||
| 9/3/09 | dfci | 10.3 | 3.9 | 35.1 | 12.0 | 428 | 13.5 | 12 | 1.24 | 74 | 11 | 31 | 742 | 1.8 | 2250 | 1.4 | 8.1/8.6 | 137 | 4.5 | 1.1 | .678 | ||||||||||||
| 10/1/09 | dfci | 9.2 | 3.97 | 35.2 | 12.1 | 475 | 13.6 | 24 | 2.21 | 60 | 13 | 29 | 694 | 1.86 | 2390 | 1.4 | 8.1/8.6 | 84 | 4.5 | 1.0 | .638 | ||||||||||||
| 10/1/09 | dfci | BMB: PERSISTENT INVOLVEMENT BY LYMPHOPLASMACYTIC LYMPHOMA Variably cellular, overall moderately hypercellular marrow (30% fat). Approximately 40% of the cellularity (25-30% of intertrabecular space) is comprised of a nodular and interstitial infiltrate of lymphocytes, lymphoplasmacytoid forms and plasma cells. Dutcher bodies are seen. Mast cells are seen. |
|||||||||||||||||||||||||||||||
| 1/7/10 | dfci | 6.5 | 3.67 | 33.2 | 11.1 | 437 | 13.7 | 17 | 1.11 | 66 | 14 | 25 | 772 | 1.82 | 2750 | 1.5 | 7.8/8.2 | 106 | 4.4 | .9 | .776 | ||||||||||||
| 1/25/10 | el camino | 7.3 | 3.48 | 31.2 | 10.7 | 340 | 13.8 | 18.7 | 1.4 | 66 | 11.6 | ||||||||||||||||||||||
| 2/12/10 | started lbh 589 clinical trial at DFCI. Initial dosage 30mg MWF | ||||||||||||||||||||||||||||||||
| 2/10/10 | dfci | 9.7 | 3.59 | 32.1 | 10.7 | 444 | 13.8 | 5.81 | 20 | 1.94 | 15 | 32 | 724 | 1.92 | 3170 | 1.5 | 8.5 | 101 | 4.7 | 2.6 | 1.1 | .816 | |||||||||||
| 2/19/10 | hawaii | 5.9 | 3.62 | 32.1 | 10.9 | 260 | 13.4 | 13 | 71 | 15 | 4.2 | ||||||||||||||||||||||
| 2/26/10 | el camino | 33.7 | 11.6 | 107 | 2065 | ||||||||||||||||||||||||||||
| 3/5/10 | el camino | 3.9 | 3.67 | 32.8 | 11.3 | 42 | 14.5 | 24 | 1.0 | 56 | 15 | ||||||||||||||||||||||
| 3/8/10 | el camino | 5.6 | 3.84 | 33.8 | 11.8 | 19 | 13.9 | 27 | 2.0 | 60 | 11 | ||||||||||||||||||||||
| 3/8/10 | el camino | platelet xfusion: 2 units. Changed lbh dosage to 20mg MWF so now platelets >180 instead of below 20! | |||||||||||||||||||||||||||||||
| 3/10/10 | el camino | 7.4 | 35 | 12 | 79 | ||||||||||||||||||||||||||||
| 3/12/10 | dfci | 7.4 | 3.77 | 33.4 | 11.5 | 87 | 15.3 | 27 | 2.0 | 49 | 23 | 42 | 778 | 1.38 | 1880 | 7.5 | 94 | 3.8 | 1.2 | ||||||||||||||
| 3/30/10 | el camino | 7.2 | 3.64 | 11.6 | 50 | 1060 | |||||||||||||||||||||||||||
| 4/15/10 | dfci | 4.4 | 3.44 | 32.2 | 11.2 | 180 | 17.8 | 29 | 692 | 1.2 | 1490 | 7.4/6.9 | 80 (fasting) | 3.7 | 1.2 | 1.16 | |||||||||||||||||
Transferred my LBH-589 clinical trial to RMCC (start of cycle #4)
| Date | Location | Pulse | BP | WBC | RBC | HCT | HGB | PLAT | RDW | ABS POLYS |
%LYMPH | LYM ABS |
NEUT % |
MONO % |
IgA | IgG | IgM SPIE | IgM Serum |
Viscosity | Iron (serum) | Transferrin (TIBC) |
Transferrin Saturation |
Tot Protein |
Glucose | Globulin | Beta2 micro |
VLDL | LDL (calc) |
HDL | Trigly cerides |
Tot Chol |
Creatinine | k/l |
| 5/11/10 | rmcc | 3.4 | 3.2 | 31.4 | 11.1 | 105 | 14.8 | 39.1 | 1.3 | 44.7 | 15.5 | 656 | 1.0 | 1735 | 1.7 | .96 | |||||||||||||||||
| stopped for a week due to tingling numbness | |||||||||||||||||||||||||||||||||
| 6/7/10 | rmcc | 6.9 | 3.13 | 31.0 | 11.2 | 285 | 12.4 | 15.7 | 1.1 | 70.3 | 12.5 | 23 | 627 | 1.3 | 2152 | 1.8 | .72 | ||||||||||||||||
| stopped for 3 weeks due to tingling and numbness on left side. Note how IgM rose to pre-dose levels in just 3 weeks. This suggests as a monotherapy, LBH just keeps you "in check"...it will not reduce your disease burden. However, in combination with Rituxan, it should do quite a bit better. | |||||||||||||||||||||||||||||||||
| 7/8/10 | rmcc | 4.5 | 3.15 | 30.5 | 10.9 | 295 | 11.1 | 22.4 | 1.0 | 64.5 | 12.1 | 1.8 | 3138 | ||||||||||||||||||||
| 8/2/10 | rmcc (start of cycle 7) | 6.2 | 3.34 | 32.3 | 11.4 | 118 | 26.2 | 1.6 | 48.1 | 23.8 | 31 | 696 | 1.5 | 2283 | 2.3 | 6.9 | 3.5 | 2.1 | 2.52 | ||||||||||||||
| 8/4/10 | el camino | BMB: flow cytometry from stanford quantified roughly 30% lymphoma/Waldenstrom's cells in the marrow. The pathologists immunohistochemistry on the core biopsy quantified the Waldentroms at about 40%. | |||||||||||||||||||||||||||||||
| 8/27/10 | el camino | 7.4 | 3.17 | 30.6 | 10.9 | 103 | 13.4 | 18 | 1.0 | 72 | 9.0 | 83 | 709 | .8 | 1149 | 2.0 | 6.6 | 152 (non fasting) | 1.0 | 1.2 | |||||||||||||
| 9/23/10 | el camino | 4.3 | 3.33 | 32 | 11.3 | 125 | 13.3 | 32.2 | 1.4 | 61.6 | 5.8 | 82 | 744 | 1.19 | 1261 | 1.9 | 7.3 | 164 | 1.3 | 1.29 | |||||||||||||
| 10/26/10 | rmcc | 3.8 | 3.27 | 32 | 10.9 | 133 | 13.2 | 39.5 | 1.5 | 39.0 | 20.5 | 36 | 761 | 1.2 | 1870 | 1.7 | 3.3 | 2.2 | 1.17 | 4.41 | |||||||||||||
| 12/2/10 | el camino prior to surgery gall bladder removal | 6.8 | 3.8 | 37.4 | 12.8 | 413 | 14.1 | 28.2 | 1.9 | 59.3 | 11.0 | 1.2 | |||||||||||||||||||||
| 1/18/11 | rmcc | 4.2 | 3.26 | 31.6 | 11.1 | 72 | 12.8 | 39.7 | 1.6 | 39.9 | 16.1 | 28 | 659 | 0.8 | 1369 | 1.6 | 2.8 | 2.3 | 1.2 | 1.85 | |||||||||||||
| 4/12/11 | rmcc | 5.1 | 3.58 | 34.5 | 12.0 | 83 | 12.8 | 36.5 | 1.8 | 47.6 | 14.6 | 33 | 718 | 0.9 | 1418 | 1.7 | 7.3 | 77 | 4.0 | 2.0 | 1.4 | ||||||||||||
| 6/6/11 | el camino | 5.1 | 3.8 | 36.6 | 13.0 | 162 | 12.8 | 21 | 1.0 | 66 | 13 | 1179 | |||||||||||||||||||||
| 7/7 | rmcc | 4.2 | 3.55 | 34.1 | 12.0 | 110 | 30 | 693 | 1.1 | 1554 | 1.7 | 6.7 | 2.3 | 1.9 | |||||||||||||||||||
| 10/28/11 | el camino | .93 | |||||||||||||||||||||||||||||||
| 12/15/11 | rmcc | 4.7 | 3.65 | 34.7 | 12.2 | 185 | 11.8 | 37.3 | 1.8 | 46.7 | 14.6 | 29 | 651 | 1.1 | 1497 | 1.7 | 6.7 | 93 | 2.3 | 1.19 | |||||||||||||
| Date | Location | Pulse | BP | WBC | RBC | HCT | HGB | PLAT | RDW | ABS POLYS |
%LYMPH | LYM ABS |
NEUT % |
MONO % |
IgA | IgG | IgM SPIE | IgM Serum |
Viscosity | Iron (serum) | Transferrin (TIBC) |
Transferrin Saturation |
Tot Protein |
Glucose | Globulin | Beta2 micro |
VLDL | LDL (calc) |
HDL | Trigly cerides |
Tot Chol |
Creatinine | k/l |
| 3/14/12 | rmcc | 5.5 | 33.5 | 11.5 | 29 | 620 | .9 | 1224 | 1.6 | ||||||||||||||||||||||||
| 8/30/12 | rmcc | 36.3 | 12.6 | 65 | 31 | 597 | .7 | 1246 | 1.7 | 2.8 | 1.7 | ||||||||||||||||||||||
| 11/28/12 | rmcc | 35.8 | 12.5 | 111 | 30 | 741 | .9 | 1354 | 1.7 | 84 | 2.6 | 1.4 | 8.2/4.1 | ||||||||||||||||||||
| 2/17/13 | rmcc | 37.2 | 13 | 94 | 37 | 762 | 1.1 | 1416 | 1.9 | 2.6 | 1.5 | 1.58 | |||||||||||||||||||||
| 5/9/13 | rmcc | 5.4 | 34.5 | 11.8 | 226 | 33 | 831 | .9 | 1307 | 1.7 | 2.6 | 1.3 | 1.97 | ||||||||||||||||||||
| 8/8/13 | rmcc | 32.5 | 11.5 | 67 | 35 | 676 | .6 | 1046 | 1.6 | 2.4 | 1.5 | 2.06 | |||||||||||||||||||||
| 1/15/14 | rmcc | 38 | 810 | 1.0 | 1498 | 2.0 | |||||||||||||||||||||||||||
| 5/19/14 | rmcc | 138 | 1.64 | ||||||||||||||||||||||||||||||
| 6/21/14 | Stanford | Started metformin for diabetes | |||||||||||||||||||||||||||||||
| 7/7/14 | rmcc | 38 | 734 | 1.0 | 1593 | 1.8 | 3.2 | ||||||||||||||||||||||||||
| 7/16/14 | village doc (after off drug for a week to raise platlets) | 31.7 | 10.9 | 333 | |||||||||||||||||||||||||||||
| 9/24/14 | rmcc | 53 | 31 | 681 | .7 | 1256 | 1.6 | 109 | |||||||||||||||||||||||||
| 11/28/14 | theranos | 32.1 | 11.5 | 53 | |||||||||||||||||||||||||||||
| 3/11/15 | rmcc | 37 | 858 | 1.1 | 1788 | 1.8 | |||||||||||||||||||||||||||
Other
| Measure | 6/6/12 | 1/31/14 | 2/25/14 | 5/19/14 | 7/7/14 | 8/1/14 | 8/20/14 (leanlabs test) |
9/11/14 (theranos) |
Notes |
| Fasting Glucose | 108 on 7/8 | 105 | 93 | 121 | |||||
| Insulin 2.6-24.9 uIU/mL = mU/L | 11.4 | 6.3 | 14.3 before 29g carbs; 2 hr after carbs 24.7 |
||||||
| LDL-C | 76 | 58 | 57 | 115 | Under 100 is good, but this is sort of meaningless. LDL-P is what matters | ||||
| HDL-C (mg/dl) | 41 | 34 | 34 | 43 | Should be above 40. Need exercise and more MUFA and PUFA. | ||||
| Triglycerides | 271 | 81 | 159 | 139 | This was unexpectedly high. the ratio between tri/HDL being >4 is typical of being insulin resistant. However, my Triglycertides are only a tiny fraction above normal. | ||||
| HbA1c % | 6.5 | 5.6 | 5.7 | 5.2 | <=5.6 is "normal" | ||||
| LDL-P | 818 | Under 1000 is great. this is the primary thing you want to get right! | |||||||
| Apo A1 | 116 | 79 to 169 normal | |||||||
| ApoB-100 | 64 mg/dL | 46 to 174 is normal. | |||||||
| Small LDL-P | 396 | should be < 527 so fine | |||||||
| Large HDL-P | 2.6 | should be >4.8 | |||||||
| LDL size | 20.3 | should be >20.5 so close. I have even mix of Pattern A and Pattern B, but particle count is low which is the most important thing. | |||||||
| HDL-P (total) | 29.2 | should be over 30.5 so close. | |||||||
| Large VLDL-P | 3.8 | should be <2.7. No clue how to fix this. | |||||||
| VLDL size | 45.8 | should be <46.6 so ok | |||||||
| HDL size | 8.9 | Should be >9.2 | |||||||
| LP-IR score | 60 | I'm insulin resistant which causes these high numbers. Want LP-IR to drop to <45 and ideally <27, so ways to go. | |||||||
| Vitamin D | 19.3 | 17.5 | 28.9 | 54.4 | the 54 was taking 3,000 IU/day but a lot of people think 50 is too high. The 28 was taking nothing. | ||||
| Albumin/Creatinine (UACR) | 5.2 | this is good. Over 30 is devastating; it means you have microalbuminuria. <17 is normal. | |||||||
| T4 (free, direct) | 1.02 | .82 to 177 ng/dL | |||||||
| TSH | 8.45 | .45 to 4.5 uIU/mL | |||||||
| BUN/Creatinine | 13.8 | 9 to 20 | |||||||
| Calcium (serum) | 8.8 | mg/dl | |||||||
| BUN | 20 | mg/dl | |||||||
| Creatinine | 1.44 | mg/dl | |||||||
| Mercury | 2.0 | 0 to 14.9 ug/L | |||||||
Note: 5.7 A1c is average glucose of 117
NOTE: During treatment, the measurement of the K/L ratio using SFLCA (Serum free light chain assays) is used to detect mildly increased levels of free light chains even when these are undetectable by SPEP (Serum immunoelectrophoresis) and IFE (Immunofixation electrophoresis). When ongoing treatment is successful, this ratio drops quickly and so docs are able to judge at an earlier stage how well the treatment is working. As I understand, response to treatment can be detected in a matter of hours to days rather than the weeks it can take for IgM levels to drop.
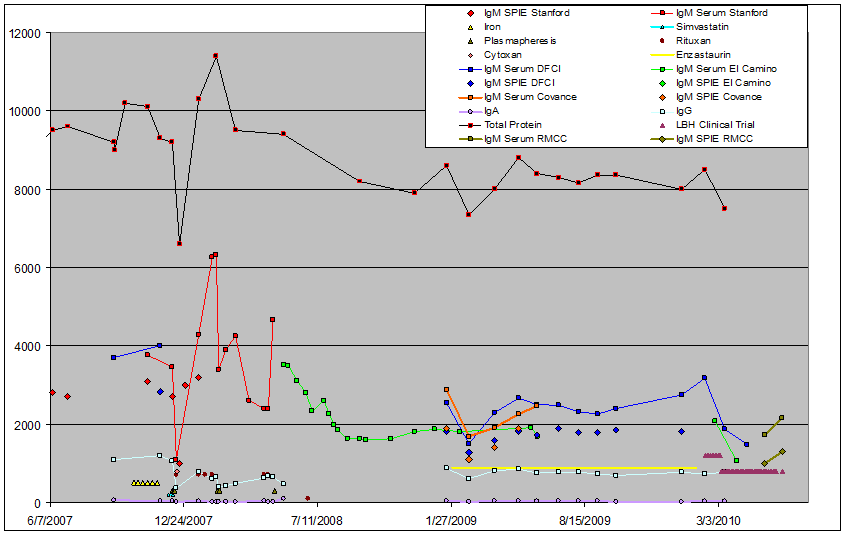
See CBC Blood Counts for a definition of terms above. Note that M-spike refers to the Serum Protein Immunofix Electrophoresis (SPIE) IgM measurement since the SPIE (aka Serum Protein Electrophoresis (SPEP)) is measuring the monoclonal spike, rather than the total serum IgM which is measured by nephlopmetry. M-spike is always less than serum IgM for that reason. M spike is normally in g/dl while serum IgM is typically measured in mg/dl. The M spike is just your "bad" IgM. If you are disease free, it should be zero. Serum IgM measures total IgM: both good and bad IgM. But the measurements are not comparable. For example, my serum IgM was at 2540 mg/dl when my kappa M spike was 1.82 g/dl. This does not mean that 1820 of the total 2540 was bad. Because they are measured two different ways, it is like comparing apples and oranges, even though they are the same (or in this case fungible) units. The correct traditional way is the SPEP as it is the one that everyone agrees is the correct way to do it.
LYM# is the absolute count or number of lymphocytes in our blood. The normal range for lymphocytes is from 1.2 to 3.4 thousand per microliter of blood and simply is cited as 1.2 to 3.4 or whatever your value may be. An average male has a volume of five liters of blood so the number of lymphocytes for that average male would be approximately 6 to 17 billion.
Beta2microglobulin is a good indicator of how fast your disease is progressing.
Normal glucose range is 70 to 150 (highest after meals). Readings consistently above 150 are a problem (see What are Normal Blood Glucose Levels).
9/11/07
Surgery at 8pm to remove my appendix. This might affect the blood counts on
9/12. The 9/11 tests were done at 9am, well before the surgery.
10/10/07: First IV iron infusion. No real side effects. Tinnitus seems a bit worse. Was tired after the infusion but that's because they didn't feed me. I was there from 9:30am to 3:30pm.
Treon thinks he may put me on CPR which is Cytoxan (an alkylating agent aka cyclophosphamide), Prednisone (a corticosteroid), rituxan which causes complete remission in 20% of patients. This is R-CVP without the V because of the peripheral neuropathy. Cyclophosphamide is well tolerated, induces minimal myelosuppression, does not deplete marrow stem cells, and is not associated with increased risk for myelodysplasia and secondary leukemia. But Cytoxan can cause kidney failure and you can develop other cancers from it. oh joy. For the cytoxan, you should drink plenty of fluids. Drink about 10 eight-ounce glasses of fluid and urinate frequently during the first 24 hours after treatment to keep your kidneys working. methotrexate has the best safety rating of the Cytotoxic drugs (see Cytoxan - Cyclophosphamide). Methotrexate can cause serious or life-threatening side effects on your liver, lungs, kidneys, and bone marrow (immune system). While Velcade could enhance the treatment, Velcade also induces neuropathies (some very serious) which is why it isn't included.
10/31/07
Did blood tests (after 3 infusions). Saw doctor. Now doing my 4th iron infusion. Also got blood tests and saw the
doctor (briefly). Based on SPIE over 7 years, my WM is growing at 13.7% per year
overall. But it grew at 14.8% in just the last 4 months (51.2% annual growth
rate). So it is now growing
MUCH faster than it has in the past. Maybe the iron infusions are helping it to
grow.
11/7/07
5th iron infusion. BP was 110/68 before infusion and 103/62 after infusion.
Heart rate was 86.
11/14/07
6th iron infusion. BP 106/65 before infusion.
11/19/07
At Dana Farber for scans, blood, and BMB. Still waiting on BMB results. 3
options: w&w, CPR + maint R, Zocor clinical trial. The idea behind taking
statins is 1) people on statins have statistically lower IgM and cholesterol
goes down in people with WM, so it could be required by the disease to grow.
Start with 20mg/day pill increasing to 80mg/day. I am 93 cholesterol now.
11/21/07
Skipped iron infusion due to plane scheduling
11/28/07
Stanford consultation: pulse 98, bp 99/61, temp 99.8
12/1/07
Began taking simvastatin on dfci clinical trial. Pills are labeled RX 791. CK
level was 25 before starting pills.
Increasing CK can indicate muscle damage.
12/5/07
Experiencing slight blurred vision in my right eye on a consistent basis (second
day). Treon told me to see an opthalmologist asap. See
Waldenstrom's Macroglobulinemia and vision problems.
12/6/07
Saw Danny Luong. Had blood spot in right eye in periphery. Such things are not
normal. Cause is generally high SV. Said SV is also causing my blurred vision.
Otherwise completely normal. Vision seems affected now on a daily basis, for
short periods (minutes). Sometimes left eye is worse and right eye is fine.
Other times it is the reverse. Treon said time to do treatment: 3 rounds of PP
(every other day), then CPR. Experiencing sharp pain for just a couple of
seconds in left rear hip. Had it happen twice. Forehead twitch happened twice
too.
12/7/07
Did first PP at 1pm. No vision problems noticed since the PP. It did leave me
tired the next day.
12/8/07
Stopped taking simvastatin.
12/9/07
Second PP at noon. Had a little trouble this time giving the machine blood at
the rate it wanted. Discovered they have a DVD/VCR library you can watch while
they PP you. This time, the blood warmer was up to temperature and put on early
(unlike last time when at first it was really cold.
12/11/07
Last round of PP completed. Hurray! They gave me my test results. Wow. The IgM
really dropped after I started taking the statin!
12/12/07
Met with Dr. Lee to clear me for chemo tomorrow. Purchased all 6 medications I'd
need (see CPR treatment details)
12/13/07 Rituxan day
Nurse was Kyla.
First chemo. They gave me oral benadryl and a few other pills before the
infusion. Rituxan is going fine so far. BP (on my leg) is 133/73 at 10:50am.
Pulse is 90. at 50mg/hr Rituxan infusion rate, no adverse reactions. 10:40am:
started rituxan at 50 rate. 11:10am: bumped it too 100. 11:12 am: stopped it
since face was feeling a little flushed (like my face was being blown up), a
little nausea; wife said face was a little pink. now giving me benadryl via iv
which will make me quite sleepy (they gave me a 25mg via pill before starting).
So now they are giving me 25mg more via IV. BP 129/69. 11:22am:
133/76. Pulse 86. 11:38am: BP is now 146/76. shivering now at 11:45am so I am
really glad i complained at the first sign of trouble, if they hadn't stopped it
when i first complained, I'm sure the shivering would be much worse! They gave
me meds IV (25 mg IV benadryl at 11:10am and 25mg IV demerol at noon to stop shaking).
stopped the infusion until the shaking was gone. 12:30: restarted at 50mg/hr.
1:02pm: Bumped up to 100 rate. I have to get 713 mg. So if I can take the 100
rate, I'm done with the rituxan by around 8pm. Nurse said 70% of people react to
rituxan first time. 1:30pm BP is 121/60. 1:33pm: bumped to 150 mg/hr.
1:45pm...feeling a tiny bit odd in back of my throat; feeling warmer this time.
2:29 upped rate to 200. 2:35pm: began feeling tingling in my chest; itchy too.
looked under my shirt: red splotches. they stopped the infusion. chest is warm.
they said it was hives. Docs don't want any more drugs put in me. Stopped
infusion at 2:35pm due to hives. It's now 2:53pm...still very itchy in front
chest, shoulders and back of neck. some splotches on my back as well. also a
small splotch on my face. 2:58pm: 10mg more IV dexamethasone (aka
decadron). will take 15
minutes to complete (I was given my first 20mg at the very start of the
treatment). Should work after 10 minutes.
Here's what my Rituxan hives look like. 3:52pm: Chest hives have almost all
gone away. Still itchy. Still some hives. I have 450mg to go. 4:13pm Hives are a
lot better. 4:17pm: Now giving me 25mg IV Benadryl to help me get rid of the
hives faster. 4:35pm, done with iv benadryl infusion. 4:42pm: most of the
hives are gone. no itchy. Just slightly on the top of my shoulders. IV benadryl
can irritate the vein during the infusion. 4:47pm: I'm back on Rituxan at
100mg/hr rate. If I get hives again, they are going to send me home. 5:20pm:
raised rate to 150mg/hr. I should have 400mg to go. BP is 115/57. this is due to
the benadryl causing drop in blood pressure. 6:21pm: itching on my head now at
the sides of my head. throbbed a little at the top of my head. 6:21pm: Stopped
infusion of Rituxan and said I was done for the day with about 200mg to go.
6:28pm: still throbbing at back top of my head. At this point, could be the rate
isn't the problem...just the total amount of drug in my body. 6:35pm: It's also
appearing under my right ear. So it is safest to stop for the day and see what
happens. They are giving me IV benadryl 25mg. (at 200mg/hr, i get benadryl burn
on the infusion; so she slowed to 150mg/hr).
Can take benadryl 25mg every 4 to six hours if I continue to have hives.
Note: I have to come back Friday for the Cytoxan since they close at 9pm. That means only 3 days prednisone at home (sat, sun, monday). 3 days for zofran starts sat (sat, sun, monday). so it's a little different from what would have happened if everything went well. Don't start any of the other medicines on Saturday.
It's not so bad I got a low total dose of Rituxan the first time. Some believe that will lead to less problems later.
12/14 check in at 10:30am
Got 250ml of cytoxan today (1900mg). temp: 98.4 bp 94/55 nurse=arturo
my BSA is 1.9 so the 1000mg/m2 is 1900 mg
11:30am started on 20mg of decadron and gave me 2 pills of (8mg per pill) of
zofran aka ondansetron
12:45pm started 250ml of cytoxan (1900mg).
1:30pm sneezed a couple of times. had to blow my nose since it was getting runny
from the infusion. eyes feel a little odd. Toward the end of the cytoxan
infusion, noticed calves are swelling. Could be constipation due to the demerol
they gave me yesterday. 14" at max.
2:49pm first glass of water after the chemo
4:15pm 2nd glass of water
5:35pm 3rd glass of water
8:25pm 4th glass of water
10pm 5th glass of water
10:30pm 6th glass of water
11:09pm 7th glass of water
12:05 bm with 3 small balls (quarter-sized diameter) plus only a little urine.
wt168.4, fat 13.7, water 61.2
12:08: after BM: wt168.2, fat 13.7, water 61.1. I'm usually 55% water, so 6%
body water increase added 10 lbs to my weight. Staring at wallpaper causes
things to move very slowly and slightly, but they move up and down a little.
Wouldn't be noticeable, except when i stared at the bathroom wallpaper. Temp is
97.3F. Talked to doc on call. Said I could take the MoM to help. Wouldn't help
urine that has to go on it's own. Said I've loaded up with plenty of water (due
to the weight gain) and not to drink anymore until i start to pass it out. I
don't have to eat unless i'm hungry (body has lots of calories it can burn).
Didn't know much about the hallucinations of things moving, but said if it got
worse, to come in.
12/18 11am
Went in due to fever of 100.3. Checked blood. My red cells have crashed so they
will give me 2 units of blood on Wednesday morning after my doctor appointment.
That should restore me to my "low" normal for a week or more.
12/19 2am
Temperature is 101.1F. Called in. No antibiotics needed since WBC counts are
high. Just take tylenol to feel better.
12/19/07 11:40am
Dr. visit. Come back in a week. If ANC<.5, get 5 Neupogen shots at stanford. If
Hct<25, get 2 units of blood. I got 1 shot of Procrit today to boost my red cell
counts, but that has most impact in 10 weeks, with little short term impact; unlike 2 units of blood
procrit starts to make a difference after 10 days. And they didn't tell me that
it increases my chance of getting leukemia; I found that out about a week after
the injection from someone who read this. You may get significant results in 30 days
according to one study (but those were WM patients): "In this study, 75.5
percent of patients (37/49) treated with PROCRIT® achieved a hematopoietic
response (HR), defined as an increase in Hb of 2 grams per deciliter (g/dL) of
blood and/or achieving a target Hb 12 g/dL during the study, independent of
blood transfusion within 28 days."
Too bad Procrit doesn't mobilize WM cells out of the marrow where they would die easier. That would have been a nice plus.
See Dr. Lee in 2 weeks from now on 1/9
Dr. advised no skiing due to altitude and low red cell counts.
12/21/07
I'm feeling OK, so I'm not going to get the 2 units of blood; I just moved
the date out a week so if my blood test on wed is low, I can still do it. I'm
much more on the conservative side now and trying to do things only if I really
need to do them since everything seems to have these side effects which I often
find out after I get the treatment.
12/27/07
Just read this paper:
Thrice-Weekly
Low-Dose Rituximab Decreases CD20 Loss via Shaving and Promotes Enhanced
Targeting in Chronic Lymphocytic Leukemia -- Williams et al. 177 (10) 7435 --
The Journal of Immunology. This suggests that just 30mg of Rituxan (20mg
of which is probably used up in clearing the cd20 cells in the bloodstream) just once a week might be quite effective in killing
my WM without any side effects and with minimal shaving (note: for me, this is
below the 20mg/m2 dose used in the paper since my BMI=2 so my dose would
normally be 40mg). It also suggests that my first treatment (about 400mg of
Rituxan) was way overkill and might be responsible for creating Rituxan-shaved
cells which then cannot be killed by Rituxan (until they regenerate their cd20)! So I may have done myself a
serious disservice. Fortunately, I didn't get the full dose! I think my body was
trying to tell me something: stop!!
1/16/08 Wednesday Infusion #1
Nurse is Gail. Blood work is moving in the right direction. Today is infusion #1
of the 4 weekly doses regimen. 20mg dexamethasone, iv 50mg benedryl, 650mg
tylenol, 20mg pepcid (via IV push). All were IV except for the tylenol. Carol
gave me an article on cytokine release syndrome. Advani examined me and said she
couldn't feel lymph nodes which is excellent news. When benedryl done, they'll
wait 30 minutes before starting me on the 713mg of Rituxan. During benedryl
infusion, my arm felt sore on the opposite side of the infusion point so they
slowed it and put a heating pack on my arm.. At 1:40pm will started the rituxan
at 25ml/hr. At 2:40pm I'm at 50ml/hr. They raised it to 125ml/hr. At 5:25pm I
feel itchy in the upperback, and also a little on the chest, top of head, back
of neck.redness in large blotches, but not really raised. 5:45pm took 2 tylenol
and got 10mg of IV dexamethasone, 25mg benedryl, and 20 mg pepcid. Restarted at
6:30pm at 75mg/ml. At 6:45, increased rate to 125mg/ml. 7:10pm: I'm still in the
clear. 9pm: reacting again so they sent me home and told me to take benadryl
when I get home
Next time I come, I am supposed to take 20mg of Prednisone the afternoon before to help reduce the infusion reactions. Taking it at night would be too close to bedtime and I'd never sleep.
Also, I should put Vaseline in my nose to keep it from getting dry which causes nosebleeds (i.e., blood when I blow my nose). Rhinaris seems to be a better long term option though (see Rhinaris - FAQ).
If rashes at home occur, can take benadryl and zantac. I took 2 benadryl (50mg total; 25 mg each), 1 zantac (150 mg) at 10pm. The rash was clear by 10:55pm.By 3am I was itchy on the scalp. At 4:18 am the itching stopped but I took 2 benadryl anyway since that is only good for 4 to 6 hours and it's been 6 hours. Didn't take another zantac since that is supposed to be good for 12 hours.
1/18/08 Friday
I'm really tired at 4pm. Go take a long nap.
1/19/08 Saturday
No energy, nausea, slight headache. Spend all day in bed I feel so weak.
1/20/08 Sunday
Slightly better today, but still feel very tired, still some nausea, headache.
Pretty much want to spend the day in bed again. Clearly this is a result of the
Rituxan treatments because I sure never felt this way before. I am taking
Levaquin for my sinusitis, but that hasn't caused nausea before, so I think it's
the Rituxan.
1/22/08 Tues
Still getting twitching in my left forefinger. That wasn't there before the
Rituxan infusions.
1/25/08 Friday Infusion #2
Nurse is Deborah.
Took 20mg Prednisone yesterday afternoon. Took 2 Claritin and 1 150mg Zantac at
8:40am.
10:30am: two Tylenol (325mg each) to stop fever that comes with Rituxan.
10:44am: now getting 20mg of decadron and 20mg Pepcid.
11:00am: now getting 50mg IV benedryl (this is double the dose they give to
people with no reaction). Had to slow it down due to slight pain on arm with
infusion
12:12pm: Rituxan started at 50mg/hr
1:15pm: Now getting 125mg/hr
4:03pm: No reactions. More than 1/2 way done. I took one more Zantac pill just
for safety since Zantac wears off after 8 hours or so.
6:40pm: Finished. No reactions.
2/5/08 Tues 3rd rituxan-only infusion (total # rituxan = 4)
Nurse is Mary. BP 110/72. Took 2 10mg Claritin and 1 150mg Zantac at 7:30am.
10:18am getting 20mg of decadron and 20mg pepcid.
10:36am: 25mg IV benadryl started. Done around 10:45am. Now waiting 30 minutes
for it to take effect before rituxan starts.
11:15am started at 50mg/hr.
11:30am BP 99/62
11:45am BP 104/62
11:51am raised to 100mg/hr for 50 ml
12:01pm BP=105/64
12:14pm BP 105/60
12:22: rate to 125mg/hr
5:40pm: done.
2/11/08 SV is 4.8. Too high. Rituxan caused the flare.
Doctor called with blood test from last Tues. SV is 4.8 and Serum IgM is 6270, i.e.,
Rituxan flare. I went in today to get another blood test taken to determine if
things are even worse. Note that I had the blood test 6 days ago! I trusted the
doctor to have called me if something was amiss. Moral of the story: the doctors
at Stanford have way too many patients to keep up with things like this. She
should have gotten the test and read it as soon as it came in. One week at high
IgM was enough to give me permanent vision loss in one eye. This was perfectly
preventable. Six key lessons that could have prevented this: 1) don't assume
your physician is on top of things 2) always always always have a blood test
before each rituxan infusion to make sure you aren't flaring since the next
infusion will make things worse 3) don't expect the hospital to do #2; you have
to insist on it; I did and it save me from a repeat of the same fiasco (see
later on), 4) keep an eye on your IgM... even if it goes down after Rituxan for
a week, you could still flare 5) get your blood test results after each test as
soon as they are available 6) if your IgM is high to start with, start with a
single PP round and a lower dose of Rituxan and see how you respond to a single
dose. Give it at least 2 weeks to see any flare. Otherwise, you are going to
have to have a LOT of PPs and it's simply not worth it. The lower dose is a much
smoother path.
2/12/08 PP day
IgM was slightly worse, SV was slightly better, but SV is not a precise test, so
in general, things over the past week are about the same. So I did one PP to get
my levels down. It isn't clear whether the spike was due to the first or second
infusion. It definitely wasn't caused by the third infusion because it was
higher before the third infusion than 1 week after it. So it was probably the
initial infusion. So one PP should get me down to safe ranges. Another option is
to take Velcade along with the Rituxan infusion as this will reduce the chance
of a flare as well as increase effectiveness. But only along with the Rituxan
since a longer course of Velcade (at least the current versions) will probably
cause very painful neuropathies. Maybe someday, that will be standard procedure.
The good news on my blood test is that Hct and Hgb are moving in the right
direction.
2/14 blood analysis
Flow cytometry on peripheral blood showed no B cells. So Rituxan completely
wiped them out.
2/15/08
Had second PP at 1pm.
So IgM lifetime is 5 days so the fact I was high means flaring is still active (just ended yesterday which is unlikely statistically). So I'm still producing IgM at this very bad rate. The 2 PP's will reduce me from 6320 to 1580, but that is no comfort at all since after 5 days, I'll be more than 63% of the final 6320 value. In short, in 5 days, I'll be at IgM 4,000 and climbing. Yuck!!!
2/16/08
Posted this update to the IWMF talklist
Several people wrote me off list asking for status updates and wondering why
I haven't posted anything recently.
So here's the quick update.
Did 4 rituxan infusions, first with cytoxan and predisone, the rest without. had
trouble with shakes and hives the first time, hives the second time, and no
reaction on the last 2 rituxan infusions.
Like 75% of people, i got a rituxan flare...serum igm skyrocketed to 6320 which
was above my pre-treatment 4,000 level. More importantly, my Serum Viscosity hit
4.8. I had ery tiny amount of retinal bleeding at SV 3.0 and my doc always does
PP whenever you exceed 4.0.
In order to restore me to lower than normal viscosity (as a contingency against
still having a flare) i had 2 PP's instead just one. The first reduced serum igm
by about half to 3390. Interestingly, the % drop in IgM is process related...i've
seen numbers that are much lower than 50% in the literature...but at Stanford
and DFCI, they always get around a 50% reduction after each PP treatment
(measured 2 days after the treatment). Don't have results on the second one, but
I'd guess a similar 50% drop.
Assuming I don't keep flaring, I won't do anything for at least a month.
I have the option of taking simvastatin to reduce my igm, but I'm worried about
it interfering with Rituxan binding and CDC per the paper at ASH. Nobody seems
to know what the active CDC "killing period" is for Rituxan for WM...is it
within the first week? first month? etc.
Going forward, I'm not yet sure what I'll do. Frequent low-dose rituxan (1/3 of
standard dose once a month) could compromise my immune system in the future.
We know that giving Velcade along with the Rituxan has a very low flare
incidence. Unlike solo rituxan, if you give both, hardly anyone flares. If used
sparingly (once a week or less), the PN of velcade is minor.
I'm leaning towards talking my doctor into going often the beaten path and doing
a 1/3 of standard dose rituxan with a Velcade once a month for a few months and
seeing how that goes. So the velcade would not be more often than once a month
and the idea is to reduce the flare but it should also aid in the killing. The
half life of velcade is short, so the impact of the velcade isn't due to the
buildup of concentration so single standard doses should work. Some docs are
worried about developing immunity to velcade if I don't follow the "standard
twice a week for N week" protocol. The 1/3 rituxan dose every month provides a
higher number of total "kill days" (where the Rituxan concentration in my body
is >25ug/ml) because Rituxan is cleared way faster in high concentrations. So 3
1/3 injections results in more Rituxan exposure than a single standard
injection.
Finally, I took 2 claritin and 1 zantac before my Rituxan infusions. They still
gave me the standard meds at the hospital, but since premedicating myself on the
morning of the treatment with those 3 pills, I've had ZERO reaction to Rituxan.
The claritin also doesn't knock you out. I could probably take a single claritin.
And there's no proof it was these pre-meds that made a difference since these
were taken on rounds 3 and 4. But the drugs are readily available and safe, and
don't make you drowsy, and they are long lasting (since my infusion was 125mg/hr
max rate i am there for 6 hours by which time all the IV meds they gave me have
long since worn off). So i'd recommend them to anyone. claritin is an H1
blocker, and zantac is an H2 blocker, so between the two of them you are
covered. The doc gave me IV benadryl and pepcid, which is the IV equivalent for
h1 and h2, but those wear off faster and I was symptom free during the whole
infusion.
2/17/08
Got an email from Arno Muller who noted the only treatment he ever had was 2 PP + 4X Rituxan. He went from:
11/19/03 Igm 8500, SV 3.9, HGB 11.
to
01/11/08 IGM 1300.
Everyone is different. The point is to give Rituxan at least 6 months to see results before trying something else. If you are lucky, the first 4 treatments are all you need. An incredible story. Others have similar stories where nothing happens for 6 months then dramatic drops.
One person reported even Velcade once every 2 weeks caused very severe PN.
So I'll do that and then maybe do RAD001 in the clinical trial at DFCI. This is an oral mtor inhibitor that seems to work pretty well in WM with few side effects.
2/18/08 Monday
I'm on a ski trip up at Beaver Creek, CO for a week. Tonight I had a
spontaneous nosebleed in my left nostril. Made a 1 inch diameter blood stain on
the pillow
2/18/08 Tues
Tonight (i.e., 12:14am Wed morning) it is the right nostril that is
spontaneously bleeding, but this time only a small drop hits the pillow before i
wake up and catch it.
While high SV can cause nosebleeds (the IgM gets in the way of the clotting), there are also nose bleeds from breathing dehydrated air at altitude which is probably what I have since I didn't have this when my IgM was really high at low altitudes (since my platlets are high). The trick is to keep your nose moist and the easiest way to do that is with a saline nasal spray, e.g., Ocean Spray, but you can also use vaseline in your nose, a humidifier, or an ointment equivalent to vaseline but without the downsides, e.g., Rhinaris If it bleeds, let it bleed out the nose. Pressure for 10 minutes works if the bleed isn't too far up your nose. Spraying Primatine Mist up your nose when it starts to bleed works well (but will sting).
4/1/08
Visual fields test at eye doctor shows I've lost some peripheral vision in one eye.
Potential causes: anemia, sleep apnea, or high SV. WM docs says she's seen it happen only for high SV. This makes sense since my SV skyrocketted to 4.8 due to the Rituxan. That was the likely cause.
4/23/08 Wed: 2nd round of Rituxan: First of 4 infusions
Nurse is Arturo.
8am: Took 2 10mg Claritin and 1 150mg Zantac right before leaving for Stanford.
They were going to give me 50mg of IV Benadryl, but I told them I had 25mg last time, so he's changing it.
Noon: 2 tylenol (650mg total), dex 20mg, pepcid 20mg, benadryl 25mg.
12:45pm: 713mg of Rituxan started at 50mg/hr.
3:21pm: feel a little queasy in my stomach. sore around my collarbone. has
been going on for at least 20 minutes so I asked them to pause the infusion.
3:50pm: Arturo insisted on restarting the infusion or I'd never finish. I
don't feel completely back to normal. I'm not sure this is a good idea. He
started it at 25mg/hr.
5:30pm: I'm back at 125mg/hr. Someone had set it to 150 for some amount of
time before that and I tolerated it just fine.
6:48pm: I increased the rate to 150mg/hr when they weren't looking.
7:08pm: I increased it to 200mg/hr. I'm almost done. At this point, the %
concentration increase is pretty small so this should be safe.
7:20pm: uh oh. noticing pain in the infusion vein. Reducing to 125mg/hr.
7:51pm: I'm done.
4/30/08 Eye doctor visit to investigate cause of my visual fields loss in
one eye
Here is msg I sent to my doctor:
had an eye exam today with Joanna Sarracino, M.D.
she said there was a change in the optic nerve shape corresponding to the visual field loss.
she speculated it could have been caused by anemia or high SV. It could also be caused by sleep apnea.
I ruled out the later since I've had sleep apnea for years and recently lost a lot of weight so it should be a lot better, yet I all of a sudden get this big field loss. Seems unlikely.
she thought i had low-pressure glaucoma, gave me the "green book" from the glaucoma research foundation, and wanted to put me on drops to lower the pressure as a precautionary measure (for the rest of my life).
Since I went through a period of low hgb and hct, and EXTREMELY high SV (4.8) right before my field loss, I'd bet it is caused by WM. And if WM is the cause, the best medicine is to fix it.
Does this sound reasonable that the WM could cause the degradation of the optic nerve causing my fields loss?
Have you had other WM patients with visual field loss after getting WM? Yes, due to high high SV.
I'm going in for a baseline test next week (on the most sensitive visual fields test they have), and we'll monitor the progress without treatment. If it progresses, we'll treat and see if that makes any difference.
4/30/08 Wed: Second of 4 infusions (second round)
12:28pm: premeds started
1:40pm Rituxan started
4:52pm Changed rate to 150 mL/hr
7:10pm: done
5/5/08 Monday
Right eye is blurry. Blinking a lot helps. It's better by Tues. Could be
indicative of IgM spike caused by 2nd Rituxan infusion.
5/7/08 Wed: 3 of 4 infusions in the second round... ABORTED
8am: Took 2 10mg Claritin and 1 150mg Zantac right before leaving for Stanford.
11am: arrived in the chair. Nurse is Carol
As I suspected,
IgM is way high: 4660 which is above where I had eye problems before. More Rituxan would be a bad thing at this point. Checking with the
doctor. Glad I asked the nurse to check first.
What's interesting is that I didn't flare at all after the first infusion (measured 1 week after infusion). But on the second infusion I had a big flare: IgM doubled in a week. This suggests that the flare is caused by peak concentration of Rituxan.
Doctor wanted me to do PP on Thurs and Friday and get next Rituxan on Sat. I think my IgM is on the decline (since my vision problems peaked on Monday), but to play it safe with my eyes, agreed to one PP.
5/8/08
9am: did one round of PP to reduce my IgM. Took 90 minutes. My vein collapsed
many times during the treatment.
5/13/08
Met with Shane Dormady at El Camino Hospital. He's willing to tailor my drug
dosing based on the measured reactions of my body rather than treating me based
on average patient response. So I'm switching. I'll get a blood test on 5/21 and
a 300mg Rituxan infusion (less than half the standard) on 5/22.
5/22/08
I'm still flaring so we'll test blood again next week. Since my body is still
reacting to the drug, presumably it must still be quite active so no need to
over do it!! In fact, since it's been 3 weeks and I'm not back to normal, it
suggests that the drug is still quite active for 3 weeks so going 4 weeks
between treatments might work quite well.
6/8/08
Still not treated yet. Testing blood every 2 weeks so next test is this
Wednesday. Will get a single green top and overnight it to do an ELISA test
using a kit from Bender MedSystems to test for sCD27. According to
Therapeutic targeting of CD70 and CD27-CD70 interactions with the monoclonal
antibody SGN-70 in Waldenstrom's Macroglobulinemia (WM) WM patients
displayed dramatically higher levels of sCD27 in their sera (median 7.45, range
0-19.42 U/ml) versus healthy donors (median 0, range 0-2.78 U/ml.
6/27/08 100mg dose day!
Nurse is Theresa. 1:30pm start time. I had pre medicated with 325 tylenol, 1
zantac, 1 claritin. Amount of Rituxan 100mg. Infusion rate started at 50, then
100, then 125. No issues.
7/3/08
Blood test shows almost 20% drop in just over a week in my IgM!!
7/28/08
IgM is now 2249. That means no flare happened for a week, then I did a mini
flare that lasted 3 week (4 weeks from infusion date). So with a standard single
dose of Rituxan, my flare lasts for 2 months. With a 100mg dose, the flare lasts
for 30 days. Ideally, I should wait until the IgM stops dropping and the flare
is gone so I can see whether the 100mg is really doing something or I am just
seeing the effects of the original infusion.
11/13/08: Referred to threatt because I complained I had to urinate frequently at night. This is likely due to diabetes and/or kidney disease.
1/20/09
Did all the blood work and BMB to qualify to enroll in the enzastaurin clinical
trial at DFCI.
1/28/09
Started enzastaurin trial today.
2/09/09
Had IgM tested at El Camino. 1812
5/8/09
My IgM went up, but I haven't been taking the pills within the 30 minute
window. You should take the pills right after your last bite, i.e., on an
optimally full stomach. So my pee color is pretty normal looking. I've asked: is
there a way to measure concentration of the drug in my body? Is pee color a
proxy for absorption? Should I take a loading dose?
10/1/09 BMB
I had a CT guided BMB which was much less painful (it was not conscious sedation). Note: for a conscious sedation BMB, you need to be fasting.
PERSISTENT INVOLVEMENT BY LYMPHOPLASMACYTIC LYMPHOMA
Variably cellular, overall moderately hypercellular marrow (30% fat).
Approximately 40% of the cellularity (25-30% of intertrabecular space) is
comprised of a nodular and interstitial infiltrate of lymphocytes,
lymphoplasmacytoid forms and plasma cells. Dutcher bodies are seen. Mast cells
are seen.
5/13/10
I was worried about my plummeting WBC and RBC under LBH-598. Dr. Dormady writes:
Only worry if your hemoglobin is less than 8.0 g/dL and if platelets are less than 20. For the white blood cells, the crucial measurement is the "absolute neutrophil count" which is the % neutrophils multiplied by your total white count. This number should be greater than 1.0. Your numbers look fine. Absolutely nothing to worry about.
6/7/10
I had numbness in my left leg and arm that spread to left part of my neck. I
stopped the LBH and the symptoms subsided. So now we are going to start up again
to see what happens. If it was drug induced, it should be symmetrical (it is
very rarely asymmetrical). It feels like my veins are popping on my left side in
my arm and near my ankle.
6/9/10
This was my last dose of LBH for a while to see if the symptoms subside
6/25/10
Met with Dr. Mark Saleh in Menlo Park, CA to discuss my tingling and
numbness symptoms that started happening after 4 months on LBH. He believes it
is caused by migraine headache which is worsened by the drug.
The reasons for his determination are as follows:
- duration of the symptoms are short lived (so it isn't MS or PN)
- the symptoms move around (so it isn't PN or spinal)
- the symptoms are below the neck and above the neck (so it isn't PN or spinal)
- I experienced severe sharp headaches when the LBH dose was 30 mg (so we have clear evidence that LBH is doing something in the brain that it doesn't like)
- My daughter said she had a migraine, but my wife never has (so possible generic disposition)
Another factor I forgot to mention is LBH caused my platelets to drop below 20 so that I had to have a transfusion of platelets. I wonder if I had some slight bleeding in the brain at that time that might have led to this or exacerbated it. So next step is to get an MRI of the brain to make sure it isn't something serious, and if I pass that, there are about 30 drugs to choose from that I can take to eliminate the symptoms and if that works, I can re start the LBH (he wants to do his drug before starting the LBH since it is a preventative rather than a treatment for an acute onset of symptoms).
7/5/10
Started on LBH again so I don't disqualify myself from the trial.
7/6/10
Brain MRI this morning to see if there is something more serious going on that
is causing the tingling, numbness.
9/21/14: Sent the following email
I am taking 2 metformin/day for diabetes, but but this isn't advised for patient with high creatinine levels. But I want to take metformin…it’s the best diabetes drug and it should be taken early when you get diabetes.
Irene said LBH-589 can cause high creatinine levels but it is temporary and caused by the drug. Is that true? That would be consistent with the inclusion criteria requiring creatinine being <1.5
Did some research today on my high creatinine levels which might be caused by LBH-589, my diabetes, or both.
http://www.medicinenet.com/diabetes_and_kidney_disease/article.htm says chronic kidney disease symptom is need to urinate frequently at night. Ah ha! Edema cause is kidney disease per simple google search.
So kidney problems è frequent urination + edema...both of which I have suffered from since my blood tests revealed diabetes and both of which I *still* suffer from.
Now let's look at my medical history:
-
· 7/07: diabetes is showing up in my blood glucose tests both at Stanford and DFCI. NOBODY realizes >140 on a random glucose is trouble because most don't know much about diabetes beyond looking at fasting levels. So my diabetes likely started before this, I just don't have the medical records handy. Creatinine is 1.2. NOBODY SAYS ANYTHING ABOUT DIABETES. Should have been a red flag...high glucose and high creatinine.
-
· 11/08: urination at night is now so bad I go to urologist complaining of this and asking what to do. Urologist can't figure it out. 2 bladder surgeries later I'm still the same. Urologist remains stumped.
-
· 1/09: random glucose is 200 at DFCI. Wow. Clear as day I'm diabetic. Nobody says anything. Creatinine 1.1.
-
· 2/10: LBH-589 trial started.
-
· 4/11: Creatinine taken at RMCC is 1.4. That's a new high! Could be caused by LBH? Or the combination of my diabetes and LBH?
-
· 6/11: get edema in my legs really bad. Irene says go to the ER at El Camino. $10,000 later they just tell me it is because I sit too much. Never happened before but this is the start of a trend. Heart function is normal. Nobody connects it to impaired kidney function.
-
· 2/13: Creatinine (at RMCC) sets a new high at 1.5
-
· 5/14: Creatinine (at RMCC) sets a new high at 1.65 (glucose at 138 which is a "between meal glucose" so should be <100)
-
· 5/14: Weiss gets a bad fasting glucose so refers me to endocrinologist at Stanford. Tests show I'm squarely a diabetic and lost all phase I insulin response.
-
· 9/14: I got tested for protein the urine. Thankfully, nothing. That would be very bad.
OK, so now I think I know the cause of my frequent urination at night and edema problems...the two problems I still have very badly that no one has been able to solve: both are caused by impaired kidney function. It is all fitting together very nicely now.
Questions:
1) will stopping the LBH-589 help my kidney numbers?
2) will lowering my blood sugar to normal levels and keeping protein intake on the low side (~50g/day) allow my kidneys to recover?
3) shouldn't I get a baseline B-12 and periodic B-12 since this is a side effect of Metformin (inhibits B-12 absorption).
4) I put Vitamin D into the normal range (54.4), but now I read that many consider this is a mistake and too high. I’m limiting now to 1000 IU/day. Since too much vitamin D causes blood calcium levels to rise, I am wondering whether I should have my serum calcium levels measured?
I will be getting a lactate meter as well to check for lactate build up periodically.
Test results scans
Stanford 7-3-07
DanaFarberTests-9-11-07
StanfordBlood-10-31-07
DanaFarberTests-11-19-07
Related articles
Waldenstrom's macroglobulinemia: Low dose Rituxan
Waldenstrom's macroglobulinemia: A new approach
Waldenstrom's macroglobulinemia:
Treatment option analysis
Waldenstrom's macroglobulinemia: CPR treatment
details (and suggested medications and pre-meds)